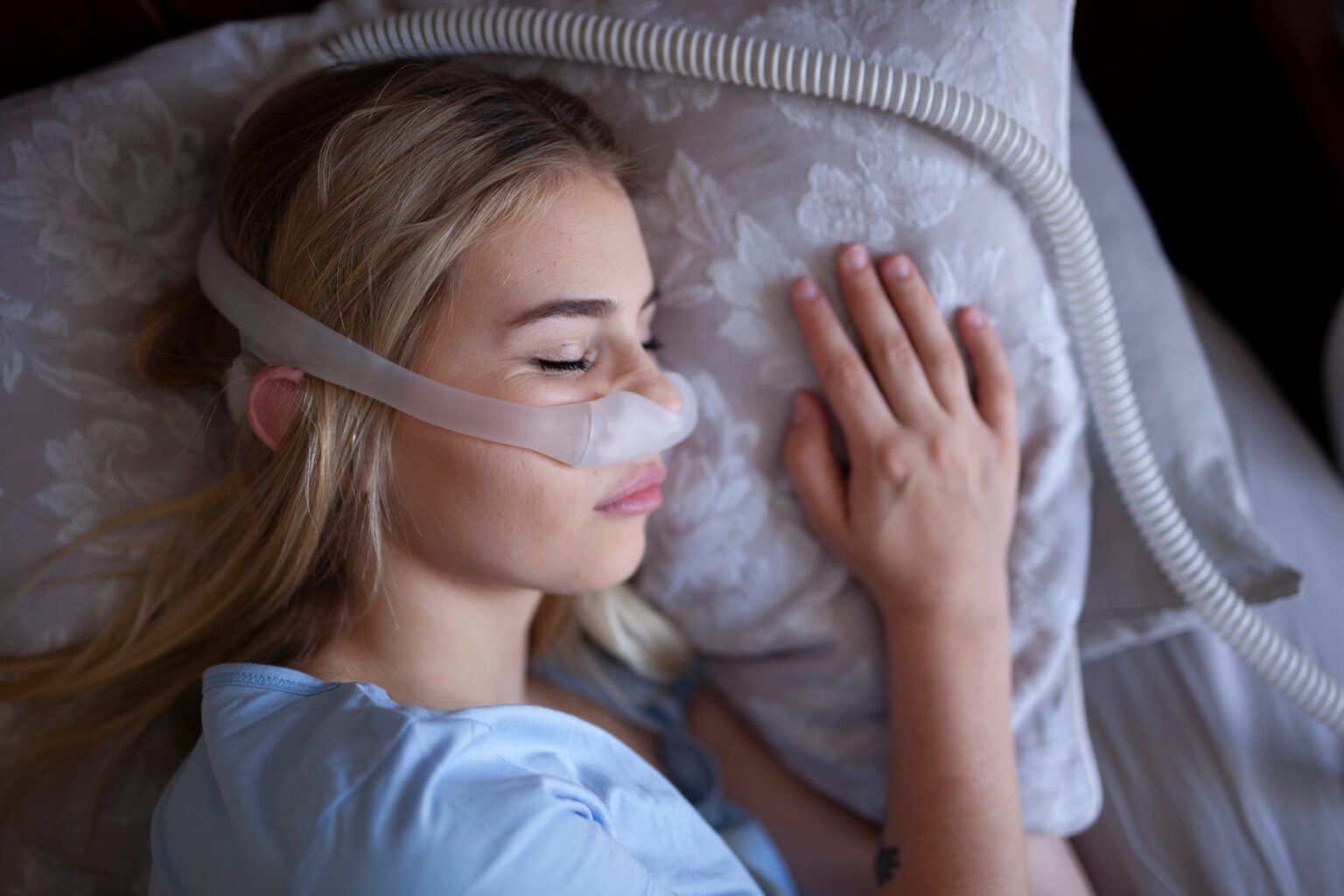
Top 3 Tips to Service Connect Sleep Apnea Secondary to PTSD Is There Really a Connection? (The
This can be helpful in allowing physicians to definitively identify whether someone has epilepsy or PNEA. Managing Stress . Whether you have PNEA or epilepsy, reducing the stress in your life can be helpful. According to the Epilepsy Foundation, 9 out of 10 people who actively manage their stress believe it has cut their risk of seizures.

Are PTSD and Sleep Apnea connected?
Pseudoseizure is an older term for events that appear to be epileptic seizures but, in fact, do not represent the manifestation of abnormal excessive synchronous cortical activity, which defines epileptic seizures. They are not a variation of epilepsy but are of psychiatric origin. Other terms used in the past include hysterical seizures, psychogenic seizures, and others. The most standard.
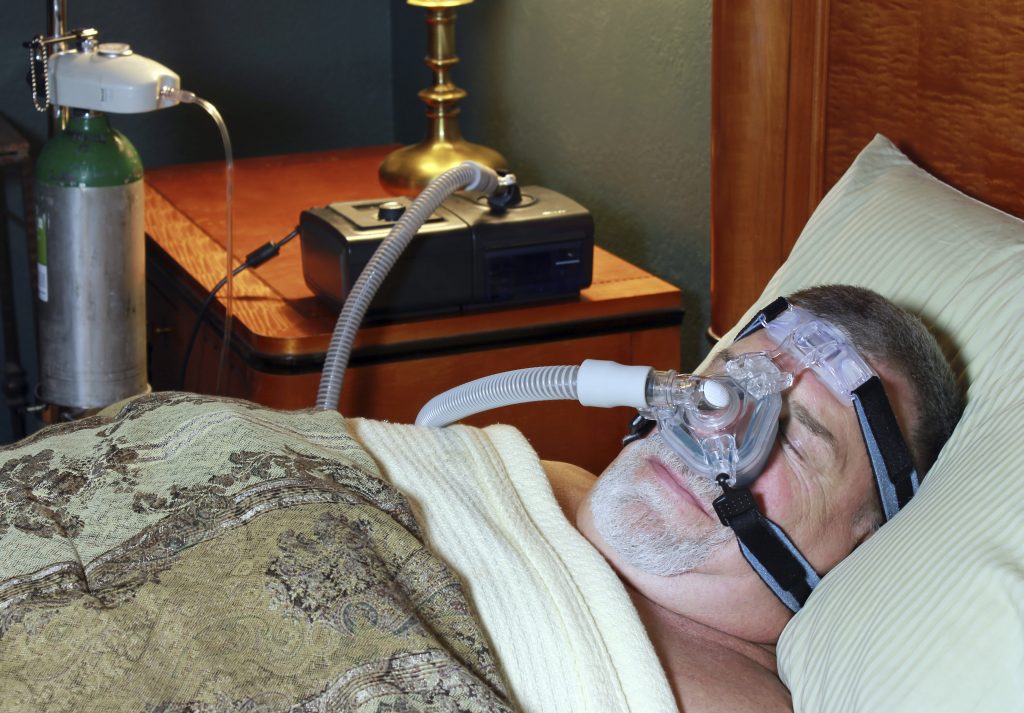
Sleep apnea and PTSD linked to poor quality of life Study
Conclusions: In the absence of a clear precipitating brain injury, approximately one in six patients intubated for emergent convulsive symptoms had PNEA rather than SE. Although PNEA cannot be diagnosed only by the presence of these risk factors, these simple characteristics could raise clinical suspicion for PNEA in the appropriate setting.
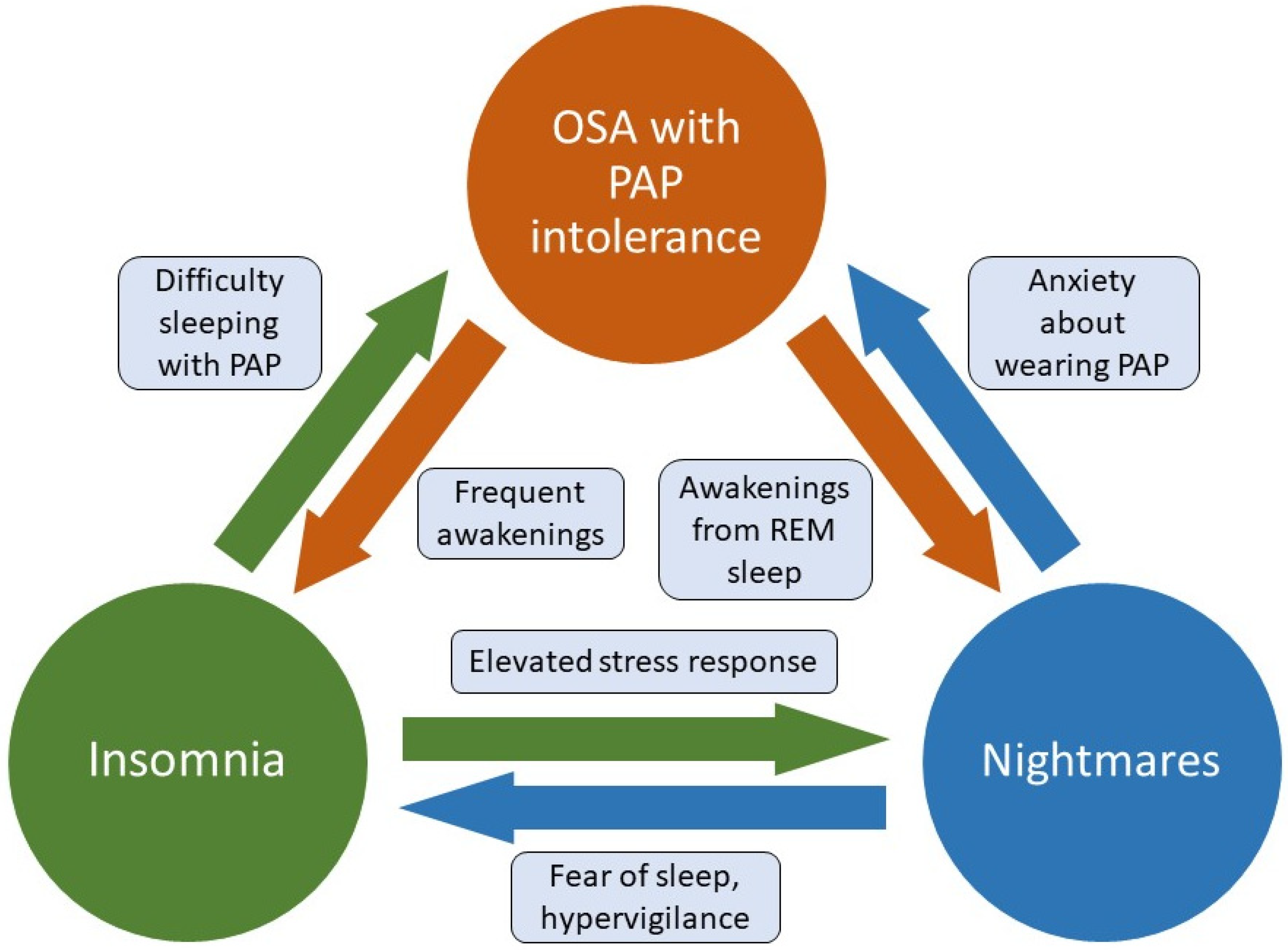
JCM Free FullText A Narrative Review of the Association between PostTraumatic Stress
Sleep-disordered breathing can be a sign of untreated OSA, which is associated with worse symptoms of PTSD, as well as an increased risk of heart failure, dementia, and certain cancers. Sleep-disordered breathing is present in 95% of individuals who evacuated a fire, and 91% of victims who experienced consecutive crimes.

The Connection Between Sleep Apnea and PTSD Sleep Foundation
Om psychogene niet-epileptische aanvallen (PNEA) te behandelen wordt in het algemeen aanbevolen dat er een goede uitleg plaatsvindt waarom er geen sprake is van een somatische aandoening, zoals epilepsie. Ook moet worden besproken wat er wel aan de hand is (psycho-educatie) (Hall-Patch et al., 2010).

How to Claim Sleep Apnea Secondary to PTSD Rep for Vets
Wetenschappelijk onderzoek bevestigt dat het onderscheid maken tussen PNEA en epilepsie één van de meest uitdagende opdrachten is voor de hulpverlener (Wood et al., 2004). Er ligt gemiddeld zeven jaar tussen de manifestatie van PNEA-klachten en het stellen van de juiste diagnose door een hulpverlener (Bodde et al., 2009b).

Top 3 Tips to Service Connect Sleep Apnea Secondary to PTSD Is There Really a Connection? (The
Psychogenic non-epileptic attacks (PNEA) are behaviors described as a sudden, violent outburst or a fit of violent action or emotion. These attacks resemble epileptic seizures, but are caused by underlying psychological factors rather than by neurological or biomedical ones. What makes PNEA different from other non-epileptic conditions, which.

Top 3 Tips to Service Connect Sleep Apnea Secondary to PTSD Is There Really a Connection? (The
Participants' self-reported PTSS rates (57.1%) were high. PTSS and pain catastrophizing, but not exposure to PTEs, were related to chronic pain severity. Interestingly, a moderated mediation analysis indicated that the indirect effect of catastrophizing in the relation between exposure to PTEs and the number of somatic symptoms via PTSS existed.

sleepapneaandptsd Tabak Law, LLC
Beyond the PTSD criterion symptoms of insomnia and nightmares, 40% to 98% of veterans with PTSD also have a co-occurring sleep disturbance such as obstructive sleep apnea (OSA), periodic leg movement disorder, sleep terrors, or nocturnal anxiety attacks. 4 - 6. OSA is one of the most common sleep disturbances, affecting between 5% and 10% of.

Sleep Apnea Secondary to PTSD? It’s time to start thinking outside the box...
Readily defined as symptoms consistent with posttraumatic stress disorder (PTSD), but that occur earlier than 30 days after experiencing the traumatic event, posttraumatic stress syndrome (PTSS) is now acknowledged to be a serious health issue. Even so, PTSS often goes unrecognized until an official.

Understanding PTSD and Sleep Apnea
Rapid side-to-side head movements. Out-of-phase limb movements. Eyes-closed unresponsiveness. Pelvic thrusting. Changing patterns of movement. As PNES is associated with psychiatric conditions, people with PNES often have co-occurring psychiatric symptoms or diagnoses, such as a depressive mood or panic attacks.

ISTSS Public Resources
Background: The empirical literature of network analysis studies of posttraumatic stress symptoms (PTSS) has grown rapidly over the last years.Objective: We aimed to assess the characteristics of these studies, and if possible, the most and least central symptoms and the strongest edges in the networks of PTSS.Method: The present systematic review, conducted in PsycInfo, Medline, and Web of.

Understanding PTSD and Sleep Apnea
Posttraumatic stress disorder (PTSD) is a debilitating anxiety disorder reported in 25% to 30% of individuals experiencing a traumatic event.1Those with this syndrome. present with constellations of symptoms such as intrusive recollection, nightmares, hyperarousal, and disturbed sleep. According to the National Comorbidity Survey, the.

Clinical Importance of Sleep Disturbance as a Treatment Target in PTSD FOCUS
Psychogenic non-epileptic attacks (PNEA) are behaviors described as a sudden, violent outburst or a fit of violent action or emotion. These attacks resemble epileptic seizures, but are caused by underlying psychological factors rather than by neurological or biomedical ones.

Sleep Apnea Secondary Connection to PTSD VA Disability Hill & Ponton, P.A.
Een functioneel-neurologisch-symptoomstoornis (FNS) is een motorische of sensorische verstoring, die niet verklaard kan worden vanuit een neurologische of andere somatische aandoening. Hierbij kan gedacht worden aan verlammingsverschijnselen, wegrakingen of abnormale schokkende bewegingen.

Oorzaken van PTSS en de risicofactoren bondig weergegeven.
Een veelvoorkomend symptoom van conversiestoornis is PNEA (Psychogene Niet-Epileptische Aanvallen)* of spanningsaanvallen. Dit betekent dat je aanvallen hebt die erg lijken op epilepsie, maar ze gaan niet samen met epileptiforme activiteit in de hersenen.